It started with what felt like a bad flu. Fever. Body aches. Tiredness. Then, within days, the lungs filled with fluid. The young man a marathon runner, perfectly healthy collapsed on the roadside in New Mexico. He was 19 years old. That was 1993. That case changed medicine forever.
Hantavirus is one of those diseases most people have never heard of until someone famous dies from it, or a new outbreak makes headlines. In early 2025, legendary Hollywood actor Gene Hackman’s wife, Betsy Arakawa, died from the virus in New Mexico. Then in May 2026, a cruise ship sailing the South Atlantic became the scene of a shocking cluster of cases, with three passengers dead and health authorities around the world on alert.
So what exactly is Hantavirus? How does it spread? Who is at risk? And what can you do to protect yourself? This guide answers every question in plain, simple English.
60–100KEstimated global cases per year
38%Case fatality rate, 2026 cruise ship outbreak
890US cases reported 1993–2023
~36%Overall US HPS death rate
What Is Hantavirus?
Hantavirus is a family of viruses carried by certain rodents mainly rats and mice. These animals carry the virus in their bodies. They shed it through their urine, droppings, and saliva. When a person breathes in tiny, invisible particles from those droppings especially in dusty or enclosed spaces they can become infected.
The virus does not make the rodent sick. But in humans, it can cause two serious diseases.
- Hantavirus Pulmonary Syndrome (HPS) mainly found in the Americas. It attacks the lungs and can cause respiratory failure.
- Hemorrhagic Fever with Renal Syndrome (HFRS) found mainly in Asia and Europe. It attacks the kidneys.
Both can be deadly. HPS has a death rate of around 36% in the United States. HFRS is generally less fatal, but still very serious.
Where Did It Come From?
The virus was not “new” in 1993. Scientists later found that hantaviruses had been circulating in rodent populations for thousands of years. In Asia and Europe, a version of the disease called HFRS had been documented as far back as the Korean War in the 1950s, when thousands of United Nations soldiers fell mysteriously ill with kidney failure.
The name “hantavirus” comes from the Hantaan River in South Korea, where an early strain the Hantaan virus was first isolated by scientists in 1978. The WHO officially named the disease “Hemorrhagic Fever with Renal Syndrome” in 1982, and the virus family was named “hantaviruses” in 1985.
But the Americas told a different story. The New World was thought to be free of dangerous hantaviruses until 1993.
A Timeline of Hantavirus in History

The 1993 Outbreak: When Everything Changed

The CDC assembled an emergency task force. Within just three weeks, scientists had identified a brand-new hantavirus eventually called Sin Nombre virus (Spanish for “No Name Virus”). The carrier was the humble deer mouse, Peromyscus maniculatus, common across the American West.
The trigger? An El Niño winter had brought unusually heavy rainfall. That caused an explosion of plants and food. The mouse population grew tenfold in one spring. More mice meant more droppings in homes, barns, and fields. More droppings meant more exposure.
By the end of 1993, 53 confirmed cases had been reported. The fatality rate was around 50%. The medical world was stunned.
Which Animals Carry Hantavirus?
- Deer mouse (USA/Canada) the main carrier of Sin Nombre virus, the deadliest North American strain
- Long-tailed pygmy rice rat (South America) carries Andes virus, the only strain known to spread between people
- Bank vole (Europe) carries Puumala virus, which causes a milder form of HFRS
- Striped field mouse (Asia) carries Hantaan virus, the original identified strain
- Common brown rat / black rat carries Seoul virus, found worldwide including in cities
Important Note
The rodents themselves never get sick from carrying the virus. They live normal lives, all while shedding the virus in their waste. You cannot tell a “safe” mouse from an infected one just by looking at it.
How Do Humans Get Infected?
This is the part most people get wrong. You do not need to touch a mouse to get hantavirus. You do not even need to see one.
The most common route is breathing. When rodent droppings, urine, or nesting materials dry out, they become dust. That dust can carry virus particles. If you breathe it in especially in a closed space like a cabin, barn, garage, or storage shed the virus can enter your body.
- Breathing in aerosols by far the most common route (sweeping old droppings, working in dusty infested areas)
- Touching contaminated surfaces, then touching your eyes, nose, or mouth
- Being bitten by an infected rodent rare, but possible
- Person-to-person only confirmed for Andes virus (South America). Most other strains, including Sin Nombre, do NOT spread this way.
Warning: The Cruise Ship Risk
In the May 2026 outbreak aboard MV Hondius, the WHO confirmed Andes virus the one strain known to spread between people. This made the situation uniquely alarming. Investigators found 8 cases and 3 deaths with a fatality rate of 38%. Six cases were lab-confirmed. Contact tracing spread across multiple countries.
Symptoms: What Does Hantavirus Feel Like?
The incubation period the time between exposure and symptoms is typically 1 to 8 weeks, though it can vary. The frightening thing about hantavirus is how ordinary it feels at first.
Early Stage (Days 1–5)
- Fever (often above 38.5°C / 101°F)
- Extreme fatigue
- Muscle aches, especially thighs and hips
- Headache
- Dizziness
- Nausea or vomiting
- Chills
Late Stage (Days 5–15)
- Sudden shortness of breath
- Dry cough
- Lungs filling with fluid
- Heart racing (tachycardia)
- Breathing rate surging
- Oxygen levels dropping rapidly
- Risk of cardiovascular collapse
The early symptoms look exactly like flu. This is the danger. Most people assume they just have a cold or fever and stay home. Then, sometimes within hours, they go from feeling unwell to fighting for their life.
“The virus gives almost no warning before it attacks the lungs. A patient can be walking and talking in the morning and on a ventilator by evening.”
How Dangerous Is Hantavirus?
Hantavirus is not “common cold” dangerous. It is “Ebola-level serious if you do not get to a hospital fast” dangerous.
- HPS (the Americas strain) kills approximately 36–50% of those infected without early hospital treatment
- HFRS (Asian/European strain) has a lower death rate typically 1–15% depending on the strain
- The 2026 cruise ship outbreak saw a 38% case fatality rate among confirmed cases
- In New Mexico from 1993–2023, 54 of 129 confirmed cases ended in death a 42% rate
- Globally, an estimated 60,000–100,000 people are infected each year, with China accounting for roughly half
Which Countries Are Most Affected?
| Region / Country | Strain | Risk Level | Notes |
|---|---|---|---|
| USA (Southwest) | Sin Nombre | High | 890 cases since 1993; New Mexico and Colorado most affected |
| Argentina / Chile / Brazil | Andes virus | High | Only strain with confirmed person-to-person spread; sharp rise since mid-2025 |
| China / South Korea | Hantaan / Seoul | High | Accounts for ~50% of global cases annually; thousands of HFRS cases yearly |
| Scandinavia / Northern Europe | Puumala | Moderate | 1,885 cases in Europe in 2023; milder HFRS; rarely fatal |
| Russia / Central Asia | Dobrava / Puumala | Moderate | Sporadic seasonal outbreaks, often rural or forested regions |
Can It Spread From Person to Person?
For most hantavirus strains including Sin Nombre, the most common US strain the answer is no. There is no confirmed evidence of person-to-person transmission for the North American strains.
But one strain is different: the Andes virus, found in South America. This is the only known hantavirus that can spread between humans. It was confirmed in the 1996–1997 Argentine outbreaks. And crucially, it is the strain behind the 2026 cruise ship cluster.
The Andes Virus Difference
In a 2018–19 Argentine outbreak study, the Andes virus had a reproductive number of about 2.12 meaning each infected person passed the virus to around 2 others before public health interventions began. After isolation and quarantine measures, that number dropped below 1, meaning the outbreak was contained.
How Do Doctors Diagnose Hantavirus?
Diagnosing hantavirus is not easy at first, because the early symptoms look so much like regular flu. Doctors usually need a combination of clinical suspicion (Has this person been in contact with rodents? Been in a rural area?) plus lab tests.
- IgM antibody blood test detects the immune response to hantavirus, usually present from the start of symptoms
- IgG antibody test a fourfold rise confirms active infection
- RT-PCR test detects hantavirus RNA directly in blood; highly accurate
- Immunohistochemical staining used in autopsy cases to detect virus antigens in tissue
- Chest X-ray shows bilateral pulmonary infiltrates (fluid in both lungs), a key diagnostic sign in HPS
Treatment Options: What Can Doctors Do?
Here is the honest, difficult truth: there is no specific approved antiviral drug for hantavirus. Doctors manage the disease, not cure it.
Treatment is what medicine calls “supportive care” keeping the patient alive while the immune system fights the virus.
- ICU admission critical for any suspected HPS case
- Supplemental oxygen often required early
- Mechanical ventilation many severe cases need a breathing machine
- ECMO (Extracorporeal Membrane Oxygenation) used in extreme cases where the lungs have failed, allowing blood to be oxygenated outside the body
- Ribavirin an antiviral drug that has been tested but not proven definitively effective for HPS; may help with HFRS in early stages
- Fluid management careful balance to avoid overloading the lungs
The Critical Window
Speed is everything. Patients who reach an ICU in the early febrile stage have a much better chance of survival than those who arrive in respiratory failure. If you have been in a rodent-exposed area and develop a sudden high fever with muscle aches, seek care immediately and tell your doctor where you have been.
Is There a Vaccine?
The short answer is: only in South Korea and it only works for Asian strains.
Hantavax was developed in 1988 and licensed by the Korean government in 1990. It protects against Hantaan and Seoul viruses. It is not approved in the US or Europe, and it does not protect against Sin Nombre or Andes virus the strains that threaten people in the Americas.
Researchers are actively developing new vaccines, particularly in the wake of the 2026 cruise ship outbreak. But as of now, there is no vaccine available for most of the world.
How Can You Protect Yourself?
At Home
- Seal any holes or gaps in your home where mice can enter even a gap the size of a dime is enough for a mouse
- Use snap traps or rodent-proof containers instead of sweeping droppings
- If you find a mouse nest, do not sweep or vacuum it dry that creates dangerous aerosols
- Wet the area first with a bleach solution (1 part bleach to 10 parts water), let it soak 5 minutes, then wipe up with gloves on
- Store food in sealed containers never leave grain or pet food open overnight
- Keep your home clutter-free mice nest in piles of cardboard, clothes, and wood
Outdoors / Rural Areas
- Do not disturb rodent burrows or nests
- When camping, sleep on elevated surfaces not directly on the ground
- Air out any cabin, barn, or shed for at least 30 minutes before entering, especially if it has been closed for months
- Do not touch dead rodents with bare hands use gloves and double-bag for disposal
- Avoid camping or working near heavy rodent activity (you will see droppings, gnaw marks, or burrows)
- Wear an N95 respirator mask if cleaning up rodent-infested areas
Safe Cleaning Protocol (CDC-Recommended)
Spray contaminated areas with bleach solution → Wait 5 minutes → Wipe up with gloved hands using disposable paper towels → Double bag waste → Wash hands thoroughly. Never sweep or vacuum dry rodent droppings in an enclosed space.
Myths vs Facts About Hantavirus
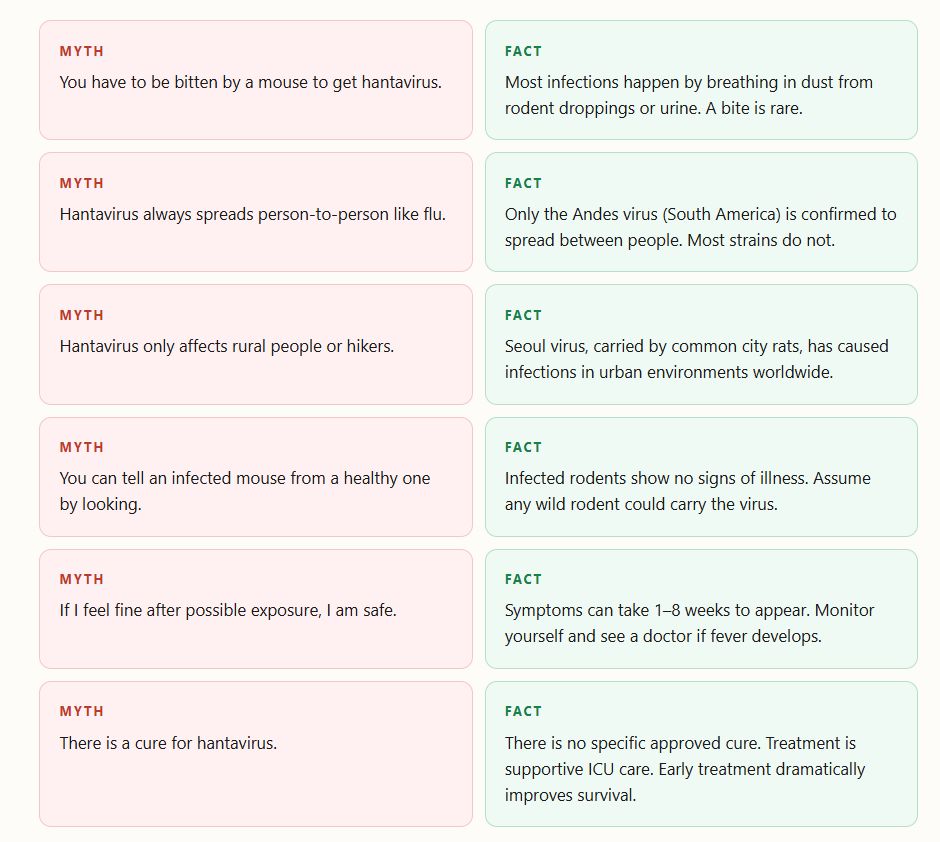

There is no specific approved cure. Treatment is supportive ICU care. Early treatment dramatically improves survival.
The 2025–2026 Resurgence: Why Now?
Scientists are not surprised that hantavirus is making headlines again. The conditions for outbreaks are getting worse, not better.
In Argentina, cases have been rising sharply. Experts point to climate change as a key factor. Unusual rainfall patterns, like the El Niño winters that triggered the 1993 outbreak, create booms in rodent populations. As humans clear forests and farmland, they move closer to rodent habitats. That means more exposure.
In Argentina alone, deaths from hantavirus reportedly rose from 28 to 101 cases between mid-2025 and early 2026. The Americas as a whole reported 299 documented cases and 59 deaths in 2025.
The cruise ship outbreak in May 2026 added a new dimension. Andes virus the person-to-person strain traveled aboard a ship from Argentina across the South Atlantic to the remote islands of Cape Verde and beyond. That is not a disease that stays in one place. That is a global risk.
WHO Risk Assessment, May 2026
The WHO stated that the risk to the global population from the cruise ship outbreak remains low. However, the organization has engaged International Health Regulations channels, and national health focal points in multiple countries are supporting contact tracing efforts. The CDC classified its hantavirus response at Level 3 its lowest emergency level as of the time of reporting.
What the Future Holds
Hantavirus research is accelerating. Scientists are working on vaccines specifically designed for New World strains especially Andes virus. The 2026 outbreak has given urgency to that work.
Antiviral drugs are also being studied more seriously. Some researchers believe monoclonal antibody therapies may eventually offer a real treatment not just supportive care.
Climate change will remain a driving force. As El Niño events become more frequent and intense, rodent population booms and the hantavirus outbreaks that follow are likely to become more common.
The best defence, for now, remains the same as it has always been: keep rodents out of your living spaces, never disturb rodent nesting areas without protection, and get to a hospital fast if you develop a mysterious fever after possible exposure.
Hantavirus is rare. But when it strikes, it moves fast. Knowledge and caution are still the best vaccines we have.
Final Word
Hantavirus will not make most of the headlines that COVID or influenza do. It is not a pandemic disease in the traditional sense. But it is a reminder of something important: nature is full of pathogens that can reach us in quiet, unexpected ways through a dusty old cabin, a mouse nest in a garage, or a passenger on a cruise ship.
A 19-year-old marathon runner in New Mexico in 1993 could not have imagined that a mouse’s dried droppings would end his life before it truly began. Betsy Arakawa, wife of one of Hollywood’s greatest actors, had no reason to suspect a virus lurking in her Santa Fe home would take her life in 2025.
This virus does not discriminate. It does not care whether you are young, old, healthy, or famous. What it responds to the only thing that consistently changes its course is preparation, awareness, and speed.
Now you know what it is. And that knowledge alone may one day save your life.
Sources & References
CDC Hantavirus Disease Reports (1993–2026) · WHO Disease Outbreak News, May 2026 · NIH/PubMed Four Corners Anniversary Study, 2018 · AJMC Hantavirus Cruise Ship Outbreak Analysis, May 2026 · CNN Health Hantavirus By the Numbers, May 2026 · UCHealth Hantavirus Precautions Feature, May 2026 · Wikipedia 1993 Four Corners Hantavirus Outbreak · Orthohantavirus Wikipedia